In today's episode of our Holding Pressure (HP) Series, developed by medical students for medical students, Janhavi and Andrew review the basics of endovascular abdominal aortic aneurysm repair (EVAR).
Authors:
Janhavi Nikhil Patel is a third and final year medical student at McMaster University. She previously completed her undergraduate in Physiology from Western University.
Andrew Lazar (@Lazar_andy) is a PGY-4 General Surgery resident at Morristown Medical Center in New Jersey. He completed a T32 research fellowship in vascular surgery at Columbia University. He graduated from Weill Cornell Medicine.
Editor: Yasong Yu
Reviewers: Imani McElroy and Amanda Fobare
Core Resources:
- Rutherford's Vascular and Endovascular Therapy 9th Edition Chapter#69, 70, 72, 73
Additional Resources:
- Relevant trials
-
- EVAR-1 Trial - In this major study out of the United Kingdom, 1252 patients with AAAs were randomly assigned to open AAA repair or EVAR. The 30 day mortality in the EVAR group was 1.8% while it was 4.3% in the open repair group. However, the early operative mortality benefit was not seen at the end of the study. There was no major difference in overall or aneurysm related mortality in the long term. EVARs were associated with increased rates of graft-related complications. Endovascular versus Open Repair of Abdominal Aortic Aneurysm. N Engl J Med, 362 (20) (2010), pp. 1863-1871
- OVER Trial - In this study of asymptomatic AAAs, patients in the Veterans Affairs system were randomized to open AAA or EVAR and followed for up to 14 years. A total of 881 patients were included with 444 getting EVAR and 437 open repair. The study demonstrated similar long term survival between operative interventions with a higher rate of secondary procedures in the EVAR arm. This study directly contraindicated two prior from Europe. F.A. Lederle, T.C. Kyriakides, K.T. Stroupe, J.A. Freischlag, F.T. Padberg, J.S. Matsumura, et al. Open versus endovascular repair of abdominal aortic aneurysm. N Engl J Med, 380 (2019), pp. 2126-2135.
Relevant Audible Bleeding episodes
- Landmark Papers - IMPROVE
- VSITE Review - AAA
- Endovascular Aortic Repair Preoperative Sizing
- VSITE Review - Vascular Access
Underlying disease featured in episode
- Pathophysiology/etiology
-
- Aneurysm means dilation of a vessel of more than 1.5x the normal arterial diameter
-
- The most common location for arterial aneurysm is the infrarenal aorta.
- The most common peripheral aneurysms are popliteal aneurysms. The most common visceral artery aneurysms are splenic artery aneurysms
- Aneurysms form from degenerative, inflammatory, infectious, genetic or traumatic processes.
-
- Degenerative - atherosclerotic disease leading to increased metalloproteinases and decreased tissue inhibitors of metalloproteinases, Smoking is the biggest risk factor for development of this type of aneurysm
- Inflammatory - fibrotic changes surrounding the aneurysm
- Infectious - variety of bacteria or fungi, including tuberculosis and syphilis
- Patients with a family history have about 30% higher chance of developing an aneurysm
- True or false aneurysms
-
- True - involve the entire vascular wall
- False - pseudoaneurysms contained hematomas surrounded by walls of connective tissue
- Prevalence of aneurysms is about 3-5x higher in men compared to women but risk of rupture is 3-fold more in women compared to men
- Patient Presentation
-
- Most patients with AAA are asymptomatic and it is discovered through incidental or surveillance imaging
-
- SVS/ESVS recommends that men 65 and older should get one-time screening ultrasound
- CSVS recommends that all men aged between 65 and 75 as well as men aged < 65 with a family history should be screened. Screening should also be done for women aged > 65 with high risk factors including smoking, cerebrovascular disease, and family history
- Some patients mention they can feel pulsations in their abdomen or if they have a smaller body habitus, can notice a pulsatile mass in the abdomen
- Diagnosis
-
- Most AAAs are recognized as a part of screening or incidental finding during either Ultrasound or a CT scan
- Duplex ultrasound is preferred given that it is non-invasive, does not require radiation, has good sensitivity and specificity to detect an aneurysm and is very affordable. However, ultrasounds have a low sensitivity and specificity to detect ruptures and can miss upto 50% of aneurysm ruptures
- For symptomatic patients, a CTA is preferred as it provides good sensitivity and specificity to detect aneurysms and ruptures. It can also provide information about vessel calcification, thrombus and concurrent arterial occlfusive disease, as well as give multi-planar and three-dimensional reconstruction of vessels
-
- Risk of exposure to radiation and the use of iodinated contrast, which limits its applicability for routine surveillance or screening.
- Treatment (Medical/Surgical)
-
- In terms of surgical options - Open or endovascular (EVAR). More than 70% of all aortic aneurysm treatment is performed with endograft technology. No clear difference in mortality in the long-term between the two procedure types.
- Indications for surgery:
-
- Aneurysms are treated at 5 cm for women and 5.5 cm for men
-
- Values are chosen because at that size, based on historical data, the risk of rupture significantly outweighed the risk of surgical intervention
- Risk of rupture in traditional studies for 5.5-6 cm aneurysms was 3.3% and for 7cm aneurysm was about 34%, however a more recent systematic review shows comparable annual risk of rupture at 5.5-6 cm of about 3.5%, but much lower risk of rupture at greater size, with > 7cm risk of 6.3% [1]
- Preop Preparation:
-
- Patients older in age, with multiple co-morbidities and would benefit more from medicine or cardiology consultation for risk optimization
- Anatomy:
-
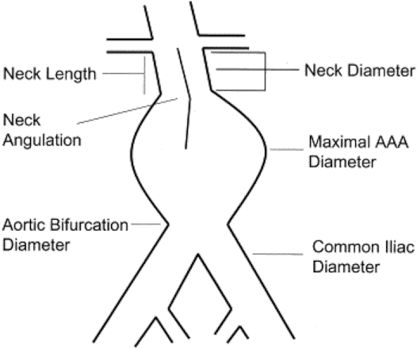
- Success in EVAR procedures greatly depend on patients vascular anatomy, as its the basis of stent device development
- Aortic neck- length, diameter, angulation and shape of the neck are important
- Minimum neck length between 5 mm to 10 mm
- Angulation between 45 to 60 degrees
- Increased angulation worse outcomes
- Neck diameter up to 32 mm
- Surgical steps with relevant images:
-
- Access to the femoral arteries can be gained either via a cutdown or percutaneous approach. Either approach leads to placement of a Guide wire in the abdominal aorta through the femoral artery
-
- The femoral artery on the side where surgeon stands is the ipsilateral site, and the opposite site is the contralateral site
- Large sheaths are placed over the wires into the aorta from both groins using fluoroscopy. Then the body graft is then slid over the guidewire of the primary side
- The graft is advanced until the top portion of the graft is positioned immediately below the renal arteries
- The aortic portion of the graft is deployed once adequate placement is confirmed. The contralateral limb gate is then cannulated with a wire. And the contralateral iliac limb is then placed. In most cases, ensuring the internal iliac artery is not covered.
-
- Although stent grafts vary, traditionally, the body of the stent graft has non-permeable polyester material with self-expanding metal frame, usually with two limbs - one for each iliac artery
- Deployment should occur with overlap sufficient to prevent leakage around the junction of the main body of the device and proximal end of limb
- The ipsilateral limb of the stent graft is deployed in similar fashion
- A balloon is then introduced and used to expand all graft to vessel and graft to graft junctions in the proximal to distal direction to ensure tight seal
- The sheaths and guide wires are removed and femoral arteries are repaired.
- Complications:
-
- Endoleaks
-
- Type I is when the blood flows into the sac around the graft proximally (1A) or distally (1B). This type of endoleak is corrected by proximal or distal device extension.
- Type II is when there is blood flow in the sac due to retrograde flow from side branches like the inferior mesenteric artery, lumbar arteries and middle sacral artery. 80% of Type II endoleaks are self-resolving with a very small rate of aneurysm rupture thus not usually treated unless sac enlargement is observed. When treated, the nidus of endoleak is embolized along with inflow and outflow vessels
- Type III is a leak between stent-graft components or from graft fabric erosions. Stent grafts can be relined or components bridged to effectively seal the defect.
- Type IV is usually due to pores in the graft fabric, noticed more commonly within 30-day of graft placement. These are self-resolving, when thrombi form at graft interstices.
- And lastly, Type V is when you have increased sac pressure "endotension" without a visible leak. If sac enlargement occurs, may need to realign with proximal or distal extension, if unsuccessful, operative explant may be needed.
- Top Asked Questions:
-
- What is the SVS guideline, who needs screening for AAA and how often?
- What is the indication for repair for AAA?
- What are the general anatomical requirements for endovascular aortic repair?
- What are the different types of endoleaks?
Calling all medical students
Submit your questions for the mailbag episode! Ask us any question related to vascular surgery, and have it answered on the podcast.
- Include the following
- Your name, school, and year
- Who you want to address the question to (resident, fellow, attending, or someone specific)
- Send them in writing, or in voice recorded format.
Send to audiblebleeding@vascularsociety.org.
Please share your feedback through our Listener Survey!
Follow us on Twitter @audiblebleeding
Learn more about us at https://www.audiblebleeding.com/about-1/ and #jointheconversation.
